Enrollment Technician
- Dignity Health Management Services
- Bakersfield, California, Remote
About Us
Inspired by faith. Driven by innovation. Powered by humankindness. CommonSpirit Health is building a healthier future for all through its integrated health services. As one of the nation’s largest nonprofit Catholic healthcare organizations, CommonSpirit Health delivers more than 20 million patient encounters annually through more than 2,300 clinics, care sites and 138 hospital-based locations, in addition to its home-based services and virtual care offerings.
Our Mission
As CommonSpirit Health, we make the healing presence of God known in our world by improving the health of the people we serve, especially those who are vulnerable, while we advance social justice for all. To learn more about a calling that defines and unites, please click here for more information about our mission, vision, and values.
The posted compensation range of $24.00 - $31.52 /hour is a reasonable estimate that extends from the lowest to the highest pay CommonSpirit in good faith believes it might pay for this particular job, based on the circumstances at the time of posting. CommonSpirit may ultimately pay more or less than the posted range as permitted by law.
- Job ID
- 2026-461936
- Employment Type
- Full Time
- Department
- Decision Support / Financial Plan
- Hours/Pay Period
- 80
- Weekly Schedule
- Monday - Friday (8:00am - 5:00pm PST)
- Shift
- Day
- Remote
- Yes
- Category
- Managed Care
Job Summary and Responsibilities
***This position may be filled as a Level I or Level II, dependent upon the final candidate's experience.
As the Enrollment Technician, you will coordinate and oversee the membership enrollment process for various health plans. This role involves reconciliation of membership data against capitation payments received from delegated health plans, assisting with enrollment issues, and supporting department goals through leadership in data integrity and workflow optimization.
Every day you will expertly assist health plans and employer groups, verify documentation, clarify program requirements, and meticulously process applications, ensuring accuracy and compliance with all established guidelines.
To be successful, you will demonstrate outstanding communication skills, strong attention to detail, and the ability to manage multiple priorities.
- Oversees the processing of enrollment and eligibility files for all lines of business, ensuring high-quality standards are maintained.
- Reconciliation of membership data against capitation payments from delegated lines of business, identifying discrepancies and implementing corrective actions.
- Acts as a primary point of contact with health plans and employer groups to resolve questions on member enrollment, including escalated issues.
- Verifies and validates data sets, such as Primary Care Physicians, effective dates, member coverage, and plan benefits, providing support to junior team members. Maintains, processes, and audits eligibility files within the database to ensure the highest levels of data integrity and accuracy.
- Supports Configuration partners (Contracting and Benefits) to streamline processes and enhance departmental efficiencies
- Develops and maintains process documentation and training materials, assisting in training new staff and mentoring junior colleagues (as a Level II).
***This position is work from home within California.
Job Requirements
Minimum Qualifications:
- 3-5+ years of experience in an administrative role with related experience (e.g., office administration support, insurance services, customer service, etc.).
- Demonstrated experience in handling complex enrollment and eligibility processes (as a Level II).
- High School diploma or GED (for Level I) or Associates Degree in a relevant field (e.g., healthcare management, business administration) or 3 years of related job or industry experience in lieu of degree (for Level II).
Preferred Qualifications:
- 3-5+ years of experience in the Managed Care/Healthcare Industry preferred.
- Experience with HMO health plans preferred.
- Experience navigating health plan portals preferred.
- Experience with EZCap preferred.
- Experience with Google Workspace a plus.
- Experience with process improvement methodologies (e.g., Lean, Six Sigma) preferred.
- Bachelors Degree in Business Administration or a related field preferred.
- Certification in Healthcare Administration or Managed Care preferred.
- Advanced Excel skills, including pivot tables, VLOOKUP, and data analysis functions.
The purpose of Dignity Health Management Services Organization (Dignity Health MSO) is to build a system-wide integrated physician-centric, full-service management service organization structure. We offer a menu of management and business services that will leverage economies of scale across provider types and geographies and will lead the effort in developing Dignity Health’s Medicaid population health care management pathways. Dignity Health MSO is dedicated to providing quality managed care administrative and clinical services to medical groups, hospitals, health plans and employers with a business objective to excel in coordinating patient care in a manner that supports containing costs while continually improving quality of care and levels of service. Dignity Health MSO accomplishes this by capitalizing on industry-leading technology and integrated administrative systems powered by local human resources that put patient care first.
Dignity Health MSO offers an outstanding Total Rewards package that integrates competitive pay with a state-of-the-art, flexible Health & Welfare benefits package. Our cafeteria-style benefit program gives employees the ability to choose the benefits they want from a variety of options, including medical, dental and vision plans, for the employee and their dependents, Health Spending Account (HSA), Life Insurance and Long Term Disability. We also offer a 401k retirement plan with a generous employer-match. Other benefits include Paid Time Off and Sick Leave.
One Community. One Mission. One California
Total RewardsDepending on the position offered, CommonSpirit Health offers a generous benefit package, including but not limited to medical, prescription drug, dental, vision plans, life insurance, paid time off (full-time benefit eligible team members may receive a minimum of 14 paid time off days, including holidays annually), tuition reimbursement, retirement plan benefit(s) including, but not limited to, 401(k), 403(b), and other defined benefits offerings, as may be amended from time to time. For more information, please visit our Total Rewards
Unless directed by a Collective Bargaining Agreement, applications for this position will be considered on a rolling basis. CommonSpirit Health cannot anticipate the date by which a successful candidate may be identified.

CommonSpirit Health™ is an Equal Opportunity/Affirmative Action employer committed to a diverse and inclusive workforce. All qualified applicants will be considered for employment without regard to race, color, religion, sex, sexual orientation, gender identity, national origin, age, disability, marital status, parental status, ancestry, veteran status, genetic information, or any other characteristic protected by law. For more information about your EEO rights as an applicant, please click here [PDF].
CommonSpirit Health™ will not discharge or in any other manner discriminate against employees or applicants because they have inquired about, discussed, or disclosed their pay or the pay of another employee or applicant. However, employees who have access to the compensation information of other employees or applicants as a part of their essential job functions cannot disclose the pay of other employees or applicants to individuals who do not otherwise have access to compensation information, unless the disclosure is (a) in response to a formal complaint or charge, (b) in furtherance of an investigation, proceeding, hearing, or action, including an investigation conducted by the employer, or (c) consistent with the contractor’s legal duty to furnish information. 41 CFR 60-1.35(c). External hires must pass a post-offer, pre-employment background check/drug screen. Qualified applicants with an arrest and/or conviction will be considered for employment in a manner consistent with federal and state laws, as well as applicable local ordinances, ban the box laws, including but not limited to the San Francisco and Los Angeles Fair Chance Ordinances. If you need a reasonable accommodation for any part of the employment process, please contact us by telephone at (415) 438-5575 and let us know the nature of your request. We will only respond to messages left that involve a request for a reasonable accommodation in the application process. We will accommodate the needs of any qualified candidate who requests a reasonable accommodation under the Americans with Disabilities Act (ADA). CommonSpirit Health™ participates in E-Verify.
-
Virtual Patient Companion
- Dignity Health
- Phoenix, Arizona
-
Education Coordinator Temporary
- Sequoia Hospital
- Redwood City, California
-
Virtual Patient Companion
- Dignity Health
- Phoenix, Arizona
-
RN, Cath Lab
- Holy Cross Hospital Jordan Valley
- West Jordan, Utah
You have not viewed any jobs yet.
You have not saved any jobs yet.
Related Content
-

News & Stories at CommonSpirit Health
Visit our News & Stories page and learn more about working at CommonSpirit Health, one of the largest nonprofit health systems in the U.S.
Learn More at News & Stories at CommonSpirit Health page -

-

-

Page Title 1
Ut enim ad minim veniam, quis nostrud exercitation ullamco laboris nisi ut aliquip ex ea commodo consequat.
Learn More at Page Title 1 page -

Page Title 2
Ut enim ad minim veniam, quis nostrud exercitation ullamco laboris nisi ut aliquip ex ea commodo consequat.
Learn More at Page Title 2 page -

Page Title 3
Ut enim ad minim veniam, quis nostrud exercitation ullamco laboris nisi ut aliquip ex ea commodo consequat.
Learn More at Page Title 3 page -

Administrative Fellowship Program
The CommonSpirit Health Administrative Fellowship is a national 18-month system-wide fellowship that offers experiential learning and exposure to strategic and operational aspects of an integrated healthcare system.
Learn More at Administrative Fellowship Program page -

Lead with humankindness - Executive Positions
Meaningful work takes a village, but inspired leadership gets it done. At CommonSpirit, our leaders influence by example and succeed through accountability. In character and conduct, you embody humankindness—by pushing us toward our best selves so we can do our best work every day.
Learn More at Lead with humankindness - Executive Positions page -

Career FAQs
Have questions about our hiring process? We're here to assist you if you're ready to apply for a position with CommonSpirit Health.
Learn More at Career FAQs page -

Our Mission and Vision
Learn about CommonSpirit Health's mission, vision and values that guide our work culture and shape our commitment to delivering humankindness.
Learn More at Our Mission and Vision page -

Military
At CommonSpirit Health, we deeply value the sacrifices made by our veterans and their families. Our commitment to supporting those who served extends beyond words—reflected in the opportunities and benefits we provide.
Learn More at Military page -

Apprenticeship Programs at CommonSpirit Health
Launch your healthcare career through our apprenticeship programs, where you can earn while you learn and gain hands-on training for a successful professional role.
Learn More at Apprenticeship Programs at CommonSpirit Health page -

Connect with a Vet
Through our Connect With a Vet program, military community members can connect one-on-one with CommonSpirit Health veterans and military spouses for personal insights into our culture, work environment, and daily life at our organization.
Learn More at Connect with a Vet page -

Interventional Radiology | CommonSpirit Health
Learn More at Interventional Radiology | CommonSpirit Health page -

National Real Estate Services at CommonSpirit Health
Explore career opportunities in real estate strategy, property management, facilities management, design and construction, and support services at CommonSpirit Health's National Real Estate Services team.
Learn More at National Real Estate Services at CommonSpirit Health page -

Our Benefits
Our benefits and perks are a big part of why we’re ranked a top employer.
Learn More at Our Benefits page -

Diversity & Inclusion
At CommonSpirit, we are dedicated to delivering humankindness. Diversity is not just an initiative, it’s the true nature of who we are.
Learn More at Diversity & Inclusion page -

Nursing
Explore more about nursing opportunities, our nursing vision and hear from our staff members.
Learn More at Nursing page -

Recent Graduate Jobs at CommonSpirit Health
Earn top-of-class work experience with a nursing leader. As a graduate with the pedigree, tech-savvy, and faith in your own destiny, you embody the next generation of healthcare. At CommonSpirit, our investment in you, personally and professionally, is how we achieve our mission, vision, and values.
Learn More at Recent Graduate Jobs at CommonSpirit Health page -

CommonSpirit Health teams up with Proxima Careers
CommonSpirit Health and Proxima Careers are partnering to expand access to healthcare careers by providing training, job placement, and ongoing support, helping community members achieve stable, well-paying jobs.
Learn More at CommonSpirit Health teams up with Proxima Careers page -

CommonSpirit Health Alumni Community
Interested in returning to CommonSpirit Health? Learn about jobs, company news, and hear from our team members.
Learn More at CommonSpirit Health Alumni Community page -

Application Notices and Information
Learn about CommonSpirit Health's application process, important notices, and requirements.
Learn More at Application Notices and Information page -

CHI Health 2026 Nursing Internship
CHI Health Nursing Internship in Nebraska
Learn More at CHI Health 2026 Nursing Internship page -

CHI Health Career Ladder CNA Program
CHI Health has partnered with local Certified Nursing Assistant Programs to offer students C.N.A. training in exchange for full or part-time employment!
Learn More at CHI Health Career Ladder CNA Program page -

Make an impact in Therapy at CommonSpirit Health
As a Physical Therapist, Occupational Therapist, or Speech-Language Pathologist, you’ll be part of a team dedicated to improving lives through relationship-based care. With opportunities across a wide range of settings, CommonSpirit Health offers the resources, support, and career growth you need to thrive—while making a difference every day.
Learn More at Make an impact in Therapy at CommonSpirit Health page -

-

CommonSpirit Health | Stepful
CommonSpirit Health is proud to partner with Stepful to connect skilled, motivated students with rewarding Allied Health career opportunities.
Learn More at CommonSpirit Health | Stepful page -

-

Flight for Life
Flight for Life® is a national leader in air medical transport, setting the standard for excellence in critical care aviation for over 50 years. We deliver hope and specialized capabilities to communities across the Rocky Mountain region and beyond.
Learn More at Flight for Life page -

-

Innovative Virtual Nursing Model
CommonSpirit has two types of virtual nurses: ones who work at a command center to help with admissions, discharges and transfers, and ones who are part of the care team, attending rounds with physicians and being available to patients at the push of the button.
Learn More at Innovative Virtual Nursing Model page -

-

COVID-19 Vaccination Requirements
COVID-19 Vaccination Requirements at CommonSpirit Health
Learn More at COVID-19 Vaccination Requirements page -

Clinical Engineering Careers at CommonSpirit Health
A career in clinical engineering offers a fulfilling blend of technology and healthcare, with the potential to make a positive impact on patient outcomes and the overall efficiency of healthcare delivery. Learn more and explore a career in clinical engineering at CommonSpirit Health.
Learn More at Clinical Engineering Careers at CommonSpirit Health page -

Careers in Environmental Services at CommonSpirit Health
Explore career opportunities in Environmental Services at CommonSpirit Health, where we provide a clean and safe environment for patients, staff, and visitors.
Learn More at Careers in Environmental Services at CommonSpirit Health page -

Radiology Careers at CommonSpirit Health
Discover fulfilling career opportunities in Imaging Services at CommonSpirit Health and play a vital role in the diagnosis and treatment of patients' care plans.
Learn More at Radiology Careers at CommonSpirit Health page -

Pursue Your Path as a Medical Assistant at CommonSpirit Health
As a Medical Assistant at CommonSpirit Health, you'll be a crucial part of the healthcare system, making a tangible difference in patients' lives. Explore this rewarding career opportunity.
Learn More at Pursue Your Path as a Medical Assistant at CommonSpirit Health page -

Elevate your career as a Surgical Tech with CommonSpirit Health
As a surgical technician at CommonSpirit Health, you will play a vital role in guaranteeing that surgical procedures are safe and successful. You will collaborate with leading surgeons and healthcare experts in cutting-edge facilities, providing our patients with the utmost care.
Learn More at Elevate your career as a Surgical Tech with CommonSpirit Health page -

Administrative Fellowship Operations Track
The CommonSpirit Health Administrative Fellowship Operations Track will provide fellows with a broad range of health care experiences at the national and local level.
Learn More at Administrative Fellowship Operations Track page -

CommonSpirit is Advancing Equitable Opportunities for Hiring and Training
CommonSpirit Health is engaged in the Healthcare Anchor Network’s Impact Workforce Commitment, an initiative to hire and train individuals who may have faced employment barriers due to low income, lack of access to education and training, and other socioeconomic challenges.
Learn More at CommonSpirit is Advancing Equitable Opportunities for Hiring and Training page -

CommonSpirit Health Hospital Medicine
Practicing hospital medicine at CommonSpirit Health offers a unique chance to serve a mission-driven organization dedicated to improving health in diverse communities. Physicians thrive in a collaborative, interdisciplinary environment that supports holistic care, innovation, and continuous growth. With a strong focus on equity and access, hospitalists help meet the needs of underserved populations and make a lasting impact.
Learn More at CommonSpirit Health Hospital Medicine page -

CHI Health Locations
Now is the perfect time to join our CHI team in one of our locations!
Learn More at CHI Health Locations page -

Los Angeles County COVID Requirements
CommonSpirit Health Locations with COVID/FLU Vaccincation Requirements
Learn More at Los Angeles County COVID Requirements page -

Meet the CommonSpirit Health Fellows
Meet our current CommonSpirit Health Fellows. This is a national, 18-month, system-wide leadership and professional development program that offers a solid foundation for future leaders through hands-on learning experiences, exposure to clinical and non-clinical aspects and mentoring from influential innovators.
Learn More at Meet the CommonSpirit Health Fellows page -

CommonSpirit Mountain Region New Grad RN Residency
Start your nursing career with our evidence-based New Grad RN Residency Program. Receive comprehensive training and support to become the nursing professional you've envisioned.
Learn More at CommonSpirit Mountain Region New Grad RN Residency page -

National Nursing New Grad Residency Program
Learn about our new grad nursing program that is nationally-standardized and evidence-based best practice for newly licensed nurses
Learn More at National Nursing New Grad Residency Program page -

Online Accessibility Notice
Online Accessibility Notice
Learn More at Online Accessibility Notice page -

Learn about our National Travel Program
Join our National Travel Program and enjoy the variety of a travel caregiver with the security of being employed by one of the largest faith-based healthcare systems in the country.
Learn More at Learn about our National Travel Program page -

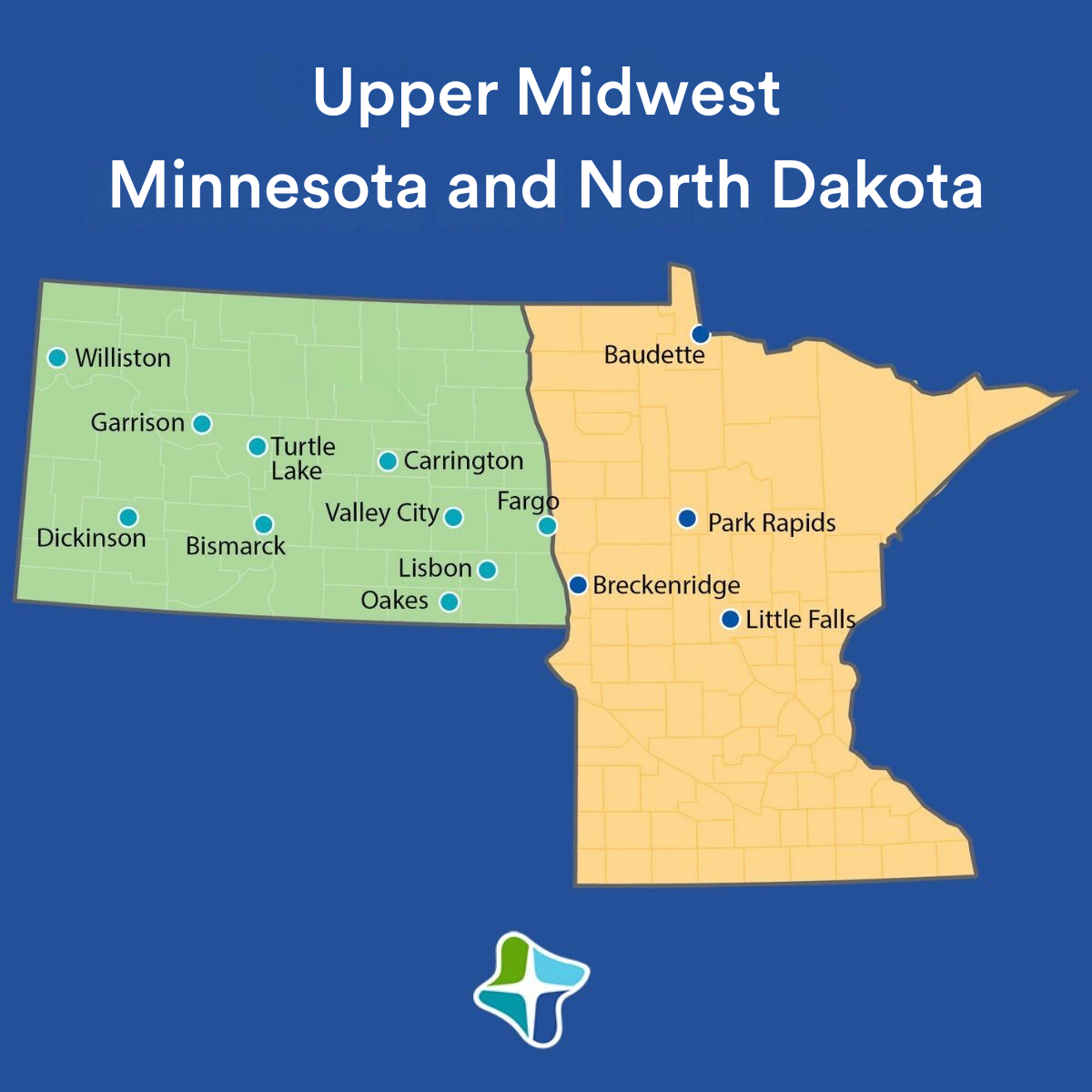
Upper Midwest
Now is the perfect time to join our healthcare team in one of our Upper Midwest locations in Minnesota and North Dakota!
Learn More at Upper Midwest page -

Learn about our Virtually Integrated Nursing Care Model
Virtually Integrated Care provides assistance to the bedside team and patient/family through the use of virtual technology.
Learn More at Learn about our Virtually Integrated Nursing Care Model page -

Virtual Command Center
Ever wondered what it was like to work in a Virtual Command Center? We’re in the background continuously assessing, reviewing and providing interventions to patients at all hours of the day across the nation.
Learn More at Virtual Command Center page -

On Demand Staffing
On Demand Staffing at CommonSpirit Health offers flexible schedules for nurses.
Learn More at On Demand Staffing page





























Share Job